Vitamin D & Hormones: The Missing Link on Every Hormone Test
Up to 1 in 5 UK adults is vitamin D deficient — and most hormone blood tests never even check for it. That's a serious blind spot. Because vitamin D isn't just a bone nutrient. It's a steroid hormone precursor that reaches into virtually every corner of your endocrine system. If it's low, your hormones feel it.
Most people who come to Vitall looking for answers about fatigue, mood swings, low libido, irregular cycles, or sluggish metabolism have already tried the basics. They've improved their sleep, cleaned up their diet, added a few supplements. And still, something feels off. Often — not always, but often — vitamin D is the thread they haven't pulled yet.
What follows is a proper look at what the research says about vitamin D's role in hormonal health, who's most at risk, what the numbers actually mean, and why our Ultimate Hormone Checks include vitamin D as a standard biomarker — when most panels quietly leave it off the list.

Wait - is vitamin D actually a hormone?
Technically, yes. The term "vitamin" is something of a historical accident. Vitamin D is synthesised in the skin via a UVB-triggered photochemical reaction, then converted in the liver to 25-hydroxyvitamin D (25(OH)D — the form we measure in blood tests), and further activated in the kidneys to its biologically potent form: 1,25-dihydroxyvitamin D, also known as calcitriol.
Calcitriol behaves like a classical steroid hormone. It binds to the vitamin D receptor (VDR) — a nuclear receptor that belongs to the same superfamily as receptors for glucocorticoids, sex hormones, and thyroid hormone (Bouillon et al., 2019; NCBI Bookshelf). And because VDR is found in tissues throughout the body — from the ovaries and testes to the adrenal glands, thyroid, brain, and immune cells — its influence extends far beyond calcium and bones.
Vitamin D speaks the same biochemical language as your sex hormones.
The vitamin D receptor (VDR) belongs to the same nuclear receptor superfamily as receptors for oestrogen, testosterone, cortisol, and thyroid hormone. When vitamin D is low, signalling across this entire receptor family can be disrupted — not just bone metabolism.
How common is vitamin D deficiency in the UK — and who's most at risk?
The UK sits at a latitude where UVB radiation is insufficient to trigger meaningful skin synthesis of vitamin D between October and March. For roughly half the year, even sunny days won't get you there. That's not a minor inconvenience — it's a structural problem that affects the whole population (UK Government; Public Health England).
According to large-scale UK Biobank analyses, approximately 17–23% of White European adults are vitamin D deficient at any given time, rising sharply in winter and spring. For people of South Asian ancestry, the figure climbs to over 57% in winter. For Black African populations, it's around 38–40% (Darling et al., 2021; Constructive et al., ScienceDirect, 2020).

The SACN (Scientific Advisory Committee on Nutrition) recommends that all UK adults consider supplementing with 10 micrograms (400 IU) of vitamin D daily, particularly from October to March. Despite this, only around 17% of UK adults regularly take supplements — suggesting a significant and largely silent deficiency is baked into the population (Donin et al., 2025).
The UK gets less sun than you think. And you can't eat your way out of it.
80–90% of our vitamin D comes from skin synthesis, not diet. Even oily fish, eggs, and fortified foods can't meaningfully compensate for six months without adequate UVB. If you've never tested your levels, the odds are your vitamin D isn't where it needs to be — especially if your hormones have been feeling off.
Where does vitamin D actually come from?
The Main Sources of Vitamin D
- Sunlight (UVB): Skin synthesis. Accounts for 80–90% of total body vitamin D. Only effective when UV index ≥ 3 (not achievable in UK Oct–Mar).
- Oily Fish: Salmon, mackerel, sardines. Rich in D3. A portion of salmon provides ~7–12 µg. Still not sufficient to correct deficiency alone.
- Eggs & Fortified Foods: Egg yolks, fortified cereals and plant milks. Low concentrations. Useful as a top-up but not a solution in isolation.
- UV-Exposed Mushrooms: Provide vitamin D2 (ergocalciferol). Less bioavailable than D3, but a plant-based option for vegans.
- Supplements (D3): Cholecalciferol (D3) is the most bioavailable form. SACN recommends 400 IU/day minimum — higher doses for deficiency.
Does vitamin D actually affect testosterone?
This is the big one for men, and the evidence is compelling. Vitamin D receptors (VDRs) are expressed in Leydig cells — the cells in the testes responsible for testosterone production. This is not a theoretical link; it's a direct mechanistic pathway. When vitamin D status is low, Leydig cell function appears to be sub-optimal (Holt et al., 2024).
A 2024 systematic review and meta-analysis published in Diseases (MDPI, Abu-Zaid et al.) searched four major medical databases and evaluated randomised controlled trials on vitamin D supplementation and male reproductive hormones. The findings pointed to significant improvements in total testosterone, free testosterone, and the free androgen index (FAI) following vitamin D supplementation in adult men. SHBG and LH were also measured as part of the picture (Abu-Zaid et al., 2024).
A complementary Danish clinical study (Holt et al., 2024, Andrology) found that vitamin D-insufficient men who received supplementation showed significantly higher testosterone-to-LH ratios compared to placebo — suggesting improved Leydig cell responsiveness. In plain English: their testes were better at converting the hormonal signal into actual testosterone.
Low vitamin D and low testosterone often travel together — and most panels only test one.
If you've had your testosterone tested and found it in the lower ranges, but nobody checked your vitamin D at the same time, you're working with an incomplete picture. The two are mechanistically linked. Checking only one is like troubleshooting your car's electrics while ignoring the battery.
What about oestrogen and progesterone — does vitamin D affect women's hormones too?
Absolutely. The VDR is present on the granulosa cells and theca cells of the ovary — the very cells responsible for producing oestrogen and progesterone. Animal studies have shown that VDR-null mice (mice without functional vitamin D receptors) have impaired folliculogenesis and lower oestrogen levels. In humans, activated vitamin D (1,25-dihydroxyvitamin D) has been shown to directly stimulate oestrogen and progesterone production in ovarian cells (Sodhi & Shah, 2019; Frontiers in Endocrinology, 2021).
A comprehensive 2021 study published in Frontiers in Endocrinology measured vitamin D alongside a full panel of female reproductive hormones — including FSH, LH, oestradiol, progesterone, testosterone, prolactin, DHEAS, SHBG, AMH, and thyroid markers — finding meaningful relationships between vitamin D status and reproductive hormone balance in reproductive-aged women. This is exactly the kind of joined-up thinking that's missing from most testing approaches.
Vitamin D has also been shown to stimulate aromatase activity — the enzyme responsible for converting testosterone into oestrogen. This has implications not just for fertility, but for hormonal balance throughout the menstrual cycle, perimenopause, and beyond.
Vitamin D may be quietly sabotaging your cycle — without you knowing.
If your periods have been irregular, your luteal phase feels off, or your progesterone hasn't quite hit the mark on testing, vitamin D status is one of the most underappreciated variables in the mix. PCOS, in particular, is strongly associated with vitamin D insufficiency — with evidence that correction can help regulate androgen levels, AMH, and menstrual patterns (Sodhi & Shah, 2019).
Can vitamin D affect cortisol and the stress response?
This one's more nuanced — and that's exactly why we're not going to oversimplify it. The relationship between vitamin D and cortisol is real but context-dependent. Here's what the evidence says.
Vitamin D receptors are expressed in the brain's stress-responsive regions — including the hypothalamus, pituitary gland, and adrenal glands — all of which are central players in the HPA (hypothalamic-pituitary-adrenal) axis, the system that governs your cortisol response (GrassrootsHealth, 2025; ScienceDirect, 2025).
A 2025 focused review in ScienceDirect confirmed that vitamin D has a significant influence on neuroendocrine regulation by modulating cortisol through both genomic and non-genomic HPA axis mechanisms. Some studies suggest cortisol levels decrease after vitamin D supplementation in cases of obesity, depression, or chronic inflammation — while effects in otherwise healthy populations are more modest. The relationship also varies with age and sex.
Additionally, research has noted that vitamin D deficiency is associated with activation of the RAAS (renin-angiotensin-aldosterone system) — a pathway involved in blood pressure regulation but also closely tied to adrenal hormone output (Frontiers in Endocrinology, 2022). Patients with Cushing's disease — characterised by excess cortisol — consistently show lower 25(OH)D levels, and the correlation between vitamin D deficiency and cortisol overproduction has been observed in multiple clinical studies.
The stress hormone your test forgot to connect the dots on.
Cortisol doesn't exist in isolation. It sits at the intersection of your immune system, blood sugar regulation, sleep-wake cycle, and reproductive hormones. When vitamin D is low, the HPA axis loses one of its regulatory inputs — meaning your cortisol rhythm may be harder to keep in check. Testing cortisol without knowing your vitamin D status is leaving an important variable out of the equation.
Is there a link between vitamin D and thyroid hormones?
Yes — and it's particularly relevant for anyone dealing with thyroid symptoms or Hashimoto's. The VDR belongs to the same nuclear receptor superfamily as the thyroid hormone receptor, and research has explored links between vitamin D status and autoimmune thyroid conditions including Hashimoto's thyroiditis and Graves' disease (Giallauria et al., 2022; Frontiers in Endocrinology).
Vitamin D's role in modulating the immune system — downregulating pro-inflammatory Th1 and Th17 cells while promoting regulatory T cells — may help reduce the autoimmune attack on thyroid tissue that characterises Hashimoto's. Several observational studies have found that people with autoimmune thyroid disease tend to have lower vitamin D levels than matched controls. Correlation isn't causation, but given the mechanistic plausibility, it's a relationship worth knowing about when you test.
The 2021 Frontiers in Endocrinology study measuring vitamin D alongside reproductive hormones in women also included free T3, T4, TSH, and TPO antibodies — reinforcing the clinical logic of looking at these biomarkers together rather than in siloed panels.
Vitamin D's Reach Across the Endocrine System
- Testosterone: VDR expressed in Leydig cells. Supplementation associated with improved total & free testosterone, FAI, and LH ratios in men.
- VDR in testes
- Oestrogen & Progesterone: VDR in granulosa & theca cells. Activated vitamin D stimulates oestrogen and progesterone synthesis in ovarian cells. Influences aromatase activity.
- VDR in ovaries
- Cortisol (HPA Axis): VDR in hypothalamus, pituitary & adrenals. Modulates HPA axis cortisol signalling via both genomic and non-genomic pathways.
- VDR in adrenals
- Thyroid Hormones: Same nuclear receptor superfamily as thyroid receptor. Vitamin D modulates immune response linked to autoimmune thyroid conditions (Hashimoto's, Graves').
- Immune regulation
- SHBG: Sex hormone-binding globulin — the protein that affects how much testosterone and oestrogen is "free" and active. Linked to vitamin D status in multiple studies.
- Transport protein
- FSH & LH: Gonadotropins that regulate the menstrual cycle and testosterone production. Studied alongside vitamin D in fertility research — part of the full picture.
- Pituitary hormones
What are the symptoms of vitamin D deficiency — and why do they look like hormone imbalance?
This is where things get genuinely tricky. The symptoms of vitamin D deficiency overlap almost perfectly with those of hormonal imbalance — which is exactly why identifying each component in isolation, through a comprehensive test, matters so much.
Symptoms commonly associated with vitamin D deficiency
- Persistent fatigue & low energy
- Low mood, depression, or anxiety
- Brain fog & poor concentration
- Muscle weakness or bone pain
- Low libido
- Irregular or absent periods
- Poor sleep quality
- Recurrent infections
- Hair thinning or loss
- Slow recovery from exercise
- Weight gain — particularly visceral
- Heightened stress sensitivity
Source: NHS; Lab Tests Online UK; GrassrootsHealth (2025). Note: these symptoms are non-specific and may have multiple causes. Testing is the only reliable way to establish vitamin D status.
What if we told you that the fatigue, brain fog, low libido, and mood dip you've been chalking up to stress - or 'just getting older' - might have a measurable, testable, addressable cause sitting quietly in your bloodwork?
So why does vitamin D keep getting left off hormone panels?
A few reasons, none of them great. Vitamin D has historically been categorised as a "bone health" nutrient, siloed into orthopaedic and geriatric medicine long before its endocrine significance was properly established. Standard GP hormone panels were designed in an era when vitamin D's receptor distribution - and its role across the endocrine system - wasn't well characterised.
The result is that you can go for a hormone test, get your testosterone, oestrogen, progesterone, LH, FSH, SHBG, cortisol, and thyroid markers all measured - and still have a deficiency quietly undermining every single one of those results. You'd never know, because nobody checked.
This is one of the most important reasons Vitall built vitamin D into our Ultimate Hormone Checks as a standard biomarker - not an optional add-on. Because you cannot meaningfully interpret a hormone panel without understanding the vitamin D status of the person you're looking at.
What should be included in a complete hormone check?
Male Ultimate Hormone Check
The most complete male hormone panel in the UK — including vitamin D, testosterone (total & free), FAI, SHBG, estrogen, cortisol, thyroid (FT4, TSH, FT3), LH, FSH, prolactin, DHEA-S, progesterone, and IGF-1.
View Male Test →Female Ultimate Hormone Check
The broadest female hormone panel in the UK — including vitamin D, estrogen, progesterone, testosterone, free testosterone, free androgen index (FAI), SHBG, cortisol, FSH, LH, prolactin, glucose, HOMA-IR, insulin, thyroid function (FT4, TSH, FT3)
What should you actually do about vitamin D?
First: test, don't guess. Symptoms are useful signals, but they're not diagnostic. The only way to know your vitamin D level is to measure it in blood - ideally as part of a comprehensive panel that also captures your hormone picture so you can see everything in context.
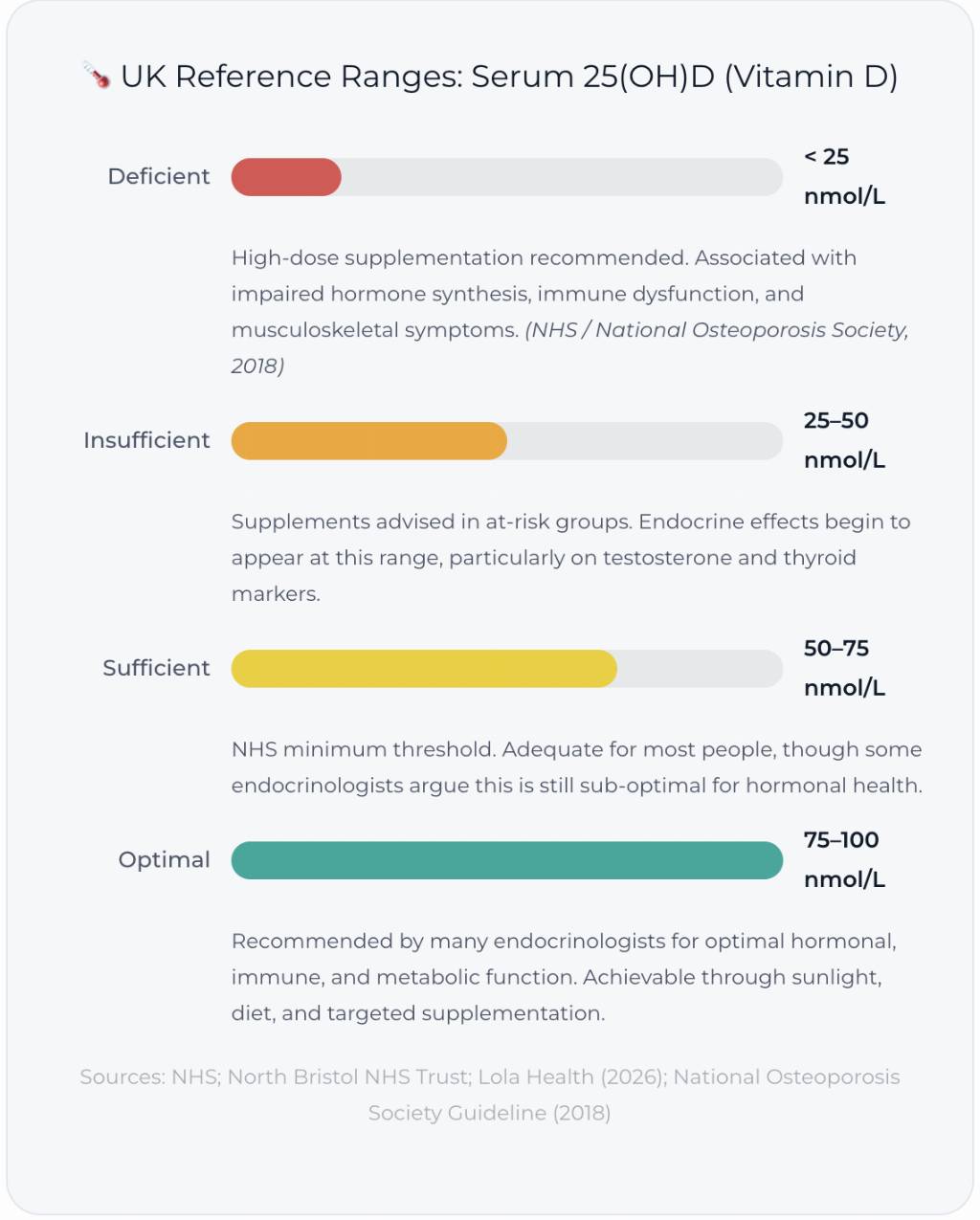
If your result comes back deficient (below 25 nmol/L), supplementation is usually recommended - typically under guidance, as the dose and duration depend on your baseline. For insufficiency (25–50 nmol/L), most people will benefit from a daily supplement of 1,000–2,000 IU (25–50 µg) of vitamin D3 (cholecalciferol), taken with a fatty meal for absorption. Vitamin K2 is often co-supplemented to support calcium directionality.
For those in the optimal range (75–100 nmol/L), maintenance supplementation of 400–1,000 IU daily through winter months is a sensible baseline. And then — retest. Because optimising without measuring is just guesswork.
Three things worth knowing before you supplement.
1. D3, not D2. Cholecalciferol (D3) raises serum 25(OH)D levels more effectively and sustainably than ergocalciferol (D2). Look for D3 in supplement form.
2. Take it with fat. Vitamin D is fat-soluble. Taking it with your largest meal of the day — or alongside a source of healthy fat — significantly improves absorption.
3. Retest after 3 months. It takes time for supplementation to move your levels. A retest at the 12-week mark gives you a proper read on whether your approach is working.
Related Guides from the Vitall Blog
- 5 Everyday Habits That Are Wrecking Your Hormones (and What to Do Instead)
- Menopause & HRT: The Complete Guide
- The 4 Seasons of Your Cycle: Female Hormonal Health
- How to Lower Cortisol Naturally: A Comprehensive Guide
- Why Am I Always Tired? The Biomarker-Led Answer to Fatigue
- The Ultimate Anti-Inflammatory Lifestyle Guide
Frequently Asked Questions
Does vitamin D affect hormone levels?
Yes. Vitamin D functions as a steroid hormone and its receptor (VDR) is found in virtually every endocrine tissue — including the testes, ovaries, adrenal glands, thyroid, hypothalamus, and pituitary. Research links adequate vitamin D levels to higher testosterone, better oestrogen and progesterone balance, improved thyroid function, and healthier cortisol rhythms.
What is a good vitamin D level for hormonal health in the UK?
The NHS considers 50 nmol/L sufficient, but many endocrinologists recommend 75–100 nmol/L for optimal hormonal function. Below 25 nmol/L is classified as deficiency and warrants clinical intervention. Vitall's Ultimate Hormone Checks measure 25(OH)D and flag results outside the optimal range.
Why is vitamin D missing from most hormone blood tests?
Vitamin D was historically categorised as a bone health nutrient, so it was siloed into separate panels. Standard hormone tests were designed before its endocrine significance was well-established. Vitall includes vitamin D in both the Male and Female Ultimate Hormone Checks as a standard biomarker, because you cannot meaningfully interpret a hormone panel without knowing the patient's vitamin D status.
Can vitamin D deficiency cause low testosterone?
Deficiency is associated with sub-optimal testosterone — not as a sole cause, but as a contributing factor. VDR is expressed in Leydig cells, and multiple RCTs have found that vitamin D supplementation in deficient men improved total testosterone, free testosterone, and free androgen index. Other factors (sleep, body composition, stress, alcohol, age) also play important roles.
Does vitamin D affect the menstrual cycle?
Evidence suggests it can. VDR is expressed on ovarian granulosa and theca cells, and activated vitamin D stimulates oestrogen and progesterone synthesis in those cells. PCOS — a condition strongly associated with hormonal irregularity — has well-established links to vitamin D insufficiency. Correction of deficiency may support cycle regularity, androgen balance, and AMH levels.
Should I take a vitamin D supplement even if I don't have symptoms?
SACN recommends that all UK adults consider 400 IU (10 µg) of vitamin D daily, particularly from October to March, regardless of symptoms. If you want to go beyond guesswork — especially if hormonal symptoms are part of your picture — testing your 25(OH)D level alongside a full hormone panel is the most informed approach.
How long does it take for vitamin D supplementation to work?
Serum 25(OH)D levels typically respond to supplementation over 8–12 weeks, with meaningful changes measurable by the 3-month mark. The dose required to reach optimal levels depends on your baseline — which is why testing before and after is the only reliable way to know your supplementation is actually working.
Get Yourself Tested With Vitall's Home Test Kits
Scientific review
Dr. Kate Bishop
Chief Scientific Officer - Vitall|Profile
Reviewed on 05/05/2026
Next review due 05/05/2027
Review focus: Blood biomarkers, laboratory testing methodology, and biochemical interpretation.
More Articles in These Categories
Similar Articles
View all articles ›References & Citations For Vitamin D & Hormones: The Missing Link on Every Hormone Test
- Abu-Zaid, A. et al. (2024). The Impact of Vitamin D on Androgens and Anabolic Steroids among Adult Males: A Meta-Analytic Review. Diseases, 12(10), 228. MDPI. DOI: 10.3390/diseases12100228.
- Bouillon, R. et al. (2019). Skeletal and Extraskeletal Actions of Vitamin D: Current Evidence and Outstanding Questions. Endocrine Reviews, 40(4), 1109–1151.
- Constructive et al. (2020). Differences and determinants of vitamin D deficiency among UK Biobank participants: a cross-ethnic and socioeconomic study. Clinical Nutrition. ScienceDirect. DOI: 10.1016/j.clnu.2020.03.019.
- Darling, A.L. et al. (2021). Very high prevalence of 25-hydroxyvitamin D deficiency in 6433 UK South Asian adults: analysis of the UK Biobank Cohort. British Journal of Nutrition. PMC7844605.
- Donin, A.S. et al. (2025). Prevalence and correlates of vitamin D deficiency in primary school children. British Journal of Nutrition. PMC7618223.
- Giallauria, F. et al. (2022). Vitamin D and adrenal gland: Myth or reality? A systematic review. Frontiers in Endocrinology, 13, 1001065. DOI: 10.3389/fendo.2022.1001065.
- GrassrootsHealth (2025). How Vitamin D Supports Stress Resilience and Mental Wellbeing. grassrootshealth.net. Accessed May 2026.
- Holt, R. et al. (2024). Effects of vitamin D on sex steroids, luteinising hormone, and testosterone to luteinising hormone ratio in 307 infertile men. Andrology, 12(3), 553–560. DOI: 10.1111/andr.13505.
- Kolberg, M.A. et al. (2021). Relationship Between Vitamin D and Hormones Important for Human Fertility in Reproductive-Aged Women. Frontiers in Endocrinology. DOI: 10.3389/fendo.2021.666687.
- NHS / North Bristol NHS Trust. Vitamin D reference ranges and treatment thresholds. nbt.nhs.uk. Accessed May 2026.
- NCBI Bookshelf. Vitamin D: Production, Metabolism, and Mechanism of Action. In: Endotext. nbk278935. Updated 2025.
- National Osteoporosis Society (2018). Vitamin D and Bone Health: A Practical Clinical Guideline for Patient Management.
- SACN (Scientific Advisory Committee on Nutrition) (2016). Vitamin D and Health. UK Government.
- ScienceDirect (2025). Vitamin D regulation of cortisol through the HPA axis: A focused review. DOI: 10.1016/j.spen.2025.000615.
- Sodhi, M. & Shah, B.C. (2019). Role of vitamin D levels on the ovarian function and androgen profile in adolescents with polycystic ovarian syndrome. Gynecology and Pelvic Medicine. DOI: 10.21037/gpm.2019.10.01.
- UK Biobank (2021). Distribution of vitamin D status in the UK: a cross-sectional analysis. PMC7789460.


